Advancing Translational Oncology with 3D Cell Culture
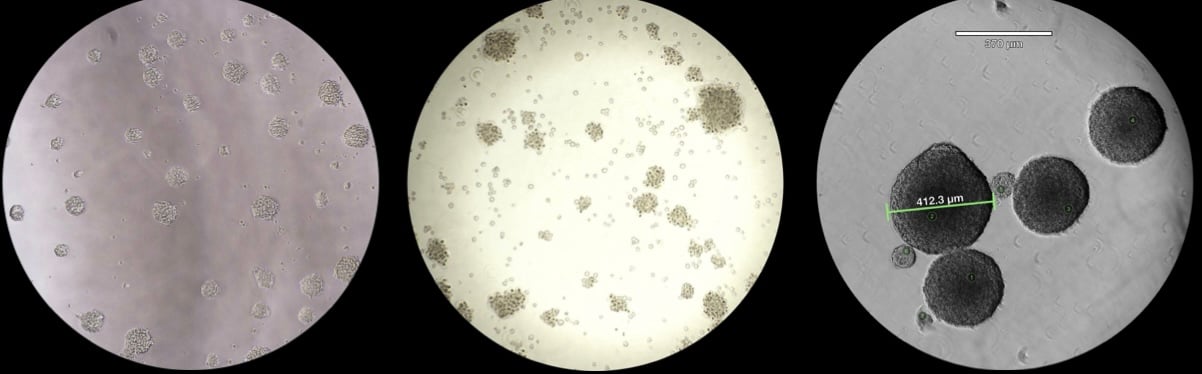
Photo Credit: Data on File. Certis Oncology (2024).
The conventional drug development pipeline has delivered incredible pharmaceutical successes and blockbusters. But, recently, appreciation for the growing number of failed drug candidates that fall by the wayside on their path to market has increased.
This translation gap is nothing new for those in translational oncology.
On the surface, we see a high failure rate for drugs transitioning from preclinical to clinical research. About 97% of drugs that enter clinical trials fail to receive FDA approval.1 This is partly due to a lack of in vitro models that accurately recapitulate the clinical characteristics of tumors. It’s time to rethink the way we approach drug discovery and development.
Fortunately, changes in cell culturing methods are improving the success rate for translational oncology. R&D and drug screening efforts have used 2D, monolayer cell cultures for basic biological and pharmacological discovery for decades. Yet, cancer is not a 2D disease. There are many facets beyond the 3D architecture of a tumor and the surrounding tumor microenvironment (TME) that simply aren’t recapitulated in monolayer cell cultures.2
This whitepaper explores the expanded use and acceptance of 3D cell cultures over 2D cell cultures in translational oncology, which may lead to more accurate pre-clinical modeling and, ultimately, better clinical outcomes. We also discuss the different types of 3D cell cultures used in cancer modeling – tumor spheroids, tumor organoids, and 3D bioprinting of tumor models – and their applications, advantages, and drawbacks in translational oncology.
2D Cell Cultures: Advantages and Limitations
Pharmaceutical and biopharmaceutical drug developers have long relied on 2D cell cultures for basic research or therapeutic efficacy, mechanisms of action (MoA), and safety/toxicity testing.
In Vitro Screens with 2D Cell Cultures. Cancer cells are bathed in a drug for a predefined period in either a glass vial or petri dish, which is not physiologically equivalent to that of a human body.
Several widely accepted benefits drove the use of 2D cell cultures. For one, they are cheap and easy to culture due to their widespread availability. Many prominent life science commercial vendors sell validated, sequenced, and heavily quality-checked cell lines, culture media, plates, and specialized equipment for 2D culturing, making the barrier to entry very low. Cell lines and suppliers have a long, established legacy in the life sciences, and given this history, pricing is affordable for most companies and research organizations.3 There have been many academic and industry publications with specific cell lines and 2D culturing conditions validating that these cell cultures can provide consistent, reproducible results. Notably, many high-throughput drug screening workflows, such as high-content analysis and flow cytometry, use 2D cell cultures for drug discovery and development.4 Cells in 2D culture also proliferate rapidly, enabling more rapid and efficient efficacy screening.2
Yet the benefits that 2D cell cultures provide drug developers – trust, validation, and ease of use – do not come without sacrifice. Adherent, monolayer growth on plastic creates a cell shape that is flat and elongated, an inherent feature of these models. 2D cells also grow in a monolayer, giving each cell the same access to nutrients, growth factors, and drugs in culture media. This creates a synchronization of the cell cycle and a lack of differentiation across the entire culture.2,5 Furthermore, cell junctions are less common in 2D cultures, reducing cell-cell communication.6 All of these 2D cell culture characteristics are non-physiological and do not accurately represent the phenotypic traits of noncancerous or cancerous cells in vivo.
Most relevant to oncology drug discovery and development, there have been many reports of the problems of 2D cell cultures in accurately predicting clinical drug responses. In a commonly used estrogen receptor (ER)-positive breast cancer cell line MCF7, for example, there was extensive genetic diversity across clones tested (n = 27 different strains), leading to changes in gene expression, cell proliferation and morphology, and highly dissimilar drug responses.7 Direct efficacy comparisons between 2D vs 3D cell cultures in models of glioblastoma, leukemia, liver, and other cancers also highlighted major deficiencies of 2D cell cultures in accurately predicting clinical efficacy.8-11 Lastly, 2D and 3D cultures' metabolic profiles are fundamentally different and change drug metabolism, which may lead to false positives or negatives in 2D cultures.12
Major Drawbacks of Using 2D Cell Cultures in Translational Oncology Include:
Changes in gene expression, cell proliferation, and morphology7
Highly dissimilar drug responses
Inaccurate clinical efficacy predictions8-11
Fundamentally different metabolic profiles, which may lead to false positives or negatives12
Smoothing the Transition from In Vitro to In Vivo: 3D Cell Culture Models
Traditionally, animal models have filled the gap left by 2D cell cultures and been more clinically- and physiologically-relevant model system for drug development. Recently, several different 3D cell culture models have become popular and closely recapitulate some of the physiological characteristics of tumors, making them more amenable to the efficacy and safety testing of oncology drugs.2
Generally, 3D cell cultures maintain several clinically relevant aspects of in vivo cell and tumor growth. First, one inherent component of the cancer model is that cells grow with 3D organization: Cells can grow in multiple layers and aggregates while maintaining natural cell shape. This creates uneven access to nutrients, oxygen, and other components of culture media and, thus, an outer layer with a high proliferation rate (because of greater access to nutrients) and an inner senescent or necrotic core (due to a hypoxic, nutrient-poor environment).2
Glioblastoma Cells Growing With 3D Organization. This 3D cell culture is derived from a 60-year-old treatment-naive female with glioblastoma. BARNEYOI® CANCER MODEL CRT00433 features an intermediate tumor mutation burden (10.66) and microsatellite instability of 5.6.
This uneven exposure and access to media and drugs closely mimic the core cells within a tumor and the surrounding tumor microenvironment. Unlike 2D cell cultures, cells grown in 3D maintain differentiated states, exhibit heterogeneous gene expression, and can communicate via gap junctions.13 This organization is linked to the greater resistance of 3D cell cultures to many therapeutics, also seen in in vivo models.14 Compared to 2D cell cultures, 3D cell cultures better recapitulate the in vivo realities of tumors, enabling drug developers to better bridge the gap between in vitro and in vivo studies.15
The Different Types of 3D Culture Systems
Several 3D cell culture models have emerged, ranging from simple to complex, and many different culturing methods – both with and without extracellular matrix (ECM) scaffolding – have been developed and detailed. Here, we’ll define two popular 3D cell culture models, tumor spheroids (also known as tumorspheres or tumoroids) and tumor organoids, highlight the major differences, and discuss 3D cell culture applications in oncology drug development.
3D Tumor Spheroids
Spheroids, also called organoid-like structures, are clusters of cells from one or more cell types that spontaneously stick together.16 The organization of these tumor spheroids and their physiological relevance depends on the source of the cells used. Cancer cell lines can create clonal cultures called multicellular tumor spheroids (MCTS), that are easy to passage and expand. Tumor spheroids can also be derived by dissociating in vivo tumor tissue samples, including brain, breast, colon, and more.17-19
TUMOR SPHEROID MODEL DEVELOPMENT AND CULTURING TECHNIQUES
Schemes of Technical Methods. (a) Pellet Culture, (b) Liquid Overlay, (c) Hanging Drop, (d) Spinner Culture, (e) Rotating Wall Vessel, (f) Microfluidics, (g) Magnetic Levitation.24
Tumor spheroids are the simplest 3D cell culture model and can be generated through cell-cell aggregation (scaffold-free methods) or cell-ECM aggregation (scaffold-based methods). Scaffold-free tumor spheroids rely on the use of gentle force to drive cell-cell adhesion. Multiple techniques have been developed to promote cell-cell aggregation, including:16
- Centrifugation: Centrifugal force is applied to a cell suspension to concentrate cells into a pellet, driving cell-cell adhesion
- Hanging drop method: Cell suspensions are applied to an inverted lid, and surface tension and gravity drive cell-cell adhesion
- Liquid overlay: Cell suspensions are applied to low adhesion plates or agar/agarose coated plates with gentle shaking or stirring. This method is amenable to 96-well or other high-throughput culturing formats.
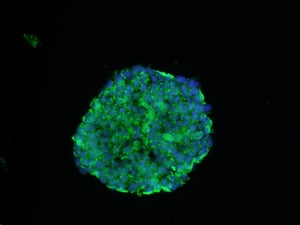 a cultured tumor spheroid in a state of hypoxia under 1% oxygen. Hypoxic areas of the spheroid are marked in green, with nuclear DIPA co-staining (blue). As tumors grow, they outpace the surrounding blood vessels' ability to provide enough oxygen, a state known as hypoxia. Rather than killing the tumor, however, hypoxia somehow triggers changes in cancer cell metabolism that allow for the tumor's continuous growth and spread into nearby tissues. Understanding more about hypoxia in cancer cells may help researchers find better ways of managing the disease. image source: NCI \ Simmons Comprehensive Cancer Center at Univ Of Texas.
a cultured tumor spheroid in a state of hypoxia under 1% oxygen. Hypoxic areas of the spheroid are marked in green, with nuclear DIPA co-staining (blue). As tumors grow, they outpace the surrounding blood vessels' ability to provide enough oxygen, a state known as hypoxia. Rather than killing the tumor, however, hypoxia somehow triggers changes in cancer cell metabolism that allow for the tumor's continuous growth and spread into nearby tissues. Understanding more about hypoxia in cancer cells may help researchers find better ways of managing the disease. image source: NCI \ Simmons Comprehensive Cancer Center at Univ Of Texas.
Each method has advantages and disadvantages and can generate tumor spheroids of different size ranges. At diameters larger than 500 µm, tumor spheroids can mimic the metabolic gradients seen in poorly or non-vascularized tumors, with an inner necrotic/hypoxic layer and an outer proliferating layer.20
Tumor spheroid applications in translational oncology
Since tumor spheroids can more accurately recapitulate aspects of in vivo solid tumor biology compared to 2D cell culture models, they are considered a more relevant in vitro model that can complement 2D monolayer testing.
Patient-derived tumor spheroid models have become particularly useful as disease-state models. Improved in vitro modeling has been accomplished for highly heterogeneous cancers, such as colorectal cancer: When multiple tumor sites are sampled to develop patient-derived spheroids, they more closely recapitulate intra-tumoral heterogeneity as compared to their 2D counterparts.21
The 3D structure of tumor spheroids also makes it possible to study the penetration and distribution of drug candidates into tumor spheroids and the viability of cells within the structure following drug exposure.22 Tumor spheroids have also been incredibly useful for drug screening and development against solid tumors. They are amenable to high-throughput, rapid screening workflows, patient-derived model development, and personalized drug testing.19,23
DrawBacks of tumor spheroids
Nonhomogenous cell clusters of varying sizes are formed for most of the tumor spheroid model development techniques.16 In addition, tumor spheroids can be fragile to handle in vitro, and sheer forces can disrupt the 3D cancer structure. Overcoming these challenges with specialized techniques can make using tumor spheroid models more standardized and reproducible.
Experimenting with different cell seeding densities in small surface areas, such as a 96-well U bottom plate, can help produce a more consistent tumor spheroid size distribution.24 Minimizing disruptions during culturing (e.g., aspirate media without disturbing tumor spheroids and performing half-media changes) and wide bore pipette tips can help preserve the 3D organization of tumor spheroids.
Tumor Organoids
Tumor organoids are more complex 3D cell culture models that consist of a mixture of organ-specific cells derived from progenitor or stem cells (e.g., adult, embryonic, or induced pluripotent stem cells) that self-assemble to mimic the organization of the tumor and organ from which they are derived.16 While organoid models can take multiple months to develop, several academic research groups have developed validated models for the brain, pancreas, ovary, and many other tumor tissues.25-27
Colorectal Cells Grown into Organoids. Microscopic image of colorectal cells grown into organoids from the foundation Hubrecht Organoid Technology (HUB), a not-for-profit organization. Using new techniques to grow cells, scientists can make models that will better resemble the tissue architecture and complexity of human tumors. Organoids are stem cell-derived human 'mini-organs' from tissues of patients with various diseases.
image SOURCE: Hubrecht Organoid Technology (HUB).
Tumor organoid model development and culturing techniques
Depending on the type of primary cells used to establish a model, tumor organoids can be used to study organogenesis, tumorogenesis, infectious diseases, and regeneration. Tumor organoids can be generated using tumor tissue and used long-term to recapitulate cellular and genetic features. There are several methods for developing tumor organoids, including the:
- Submerged method: Tissue-specific growth factor cocktails are added for culturing of tumor organoids, and organoids are grown embedded in a basement membrane scaffold with liquid media. These models are limited to epithelial cells and do not include stromal cells.
- Air-Liquid interface method: Tissue is embedded in a collagen layer, open to the air, and has access to culture media via a porous membrane beneath the tumor organoid. This model can include stromal cells and closely recapitulate the organization of the tumor microenvironment.28
- Bioreactor method: Tissue is embedded in a basement membrane and transferred to a spinning bioreactor to facilitate even distribution of nutrients and oxygen. This method had recently been applied to glioblastoma organoid growth, retaining many of the cellular and molecular features of the original tumor.25
Tumor organoid APPLICATIONS in translational oncology
Tumor organoids are advanced models for closely recapitulating the organization of the tumor microenvironment and are generally regarded as a complement to in vivo animal testing.29 Like tumor spheroids, tumor organoids are also amenable to high-throughput drug and safety testing.30 Notably, tumor organoids address challenges associated with in vivo models, such as PDXs, where limitations, such as immunotherapeutics testing, may arise.
The establishment of tumor organoid biobanks further enables the creation of reproducible cancer models, enhancing the reliability of disease modeling and drug screening protocols.31 Moreover, the alternative method of implanting tumor organoids into mice offers a practical and versatile substitute for the conventional implantation of tumor tissue biopsy, adding to the adaptability and effectiveness of this innovative approach in preclinical investigations.
drawbacks of Tumor organoids
While tumor organoids can closely recapitulate the structure of the TME, they face many of the same drawbacks as tumor spheroid models mentioned above.16 In addition, they are expensive, and can take months to establish and validate a model. The method used for model establishment and media composition can also affect experimental outcomes, putting significant pressure on using a pre-established, well-validated model for drug development. There is a significant effort to improve reporting standards and eliminate the use of reagents with high batch-to-batch variability so that tumor organoids can be more reliably cultured and used.32
the future of 3d cell culture
New techniques and technologies, such as 3D bioprinting and several microfluidics platforms, are complementing the use of 3D cell cultures in pre-clinical cancer research and drug development.
3D Bioprinting of tumor models
3D bioprinting is an innovative technique where the position of specific cells can be carefully controlled and deposited to create a pre-defined organization. 3D bioprinters use several distinct biomaterials to create these structures by using temperature or light, enzymes, or chemical crosslinking.15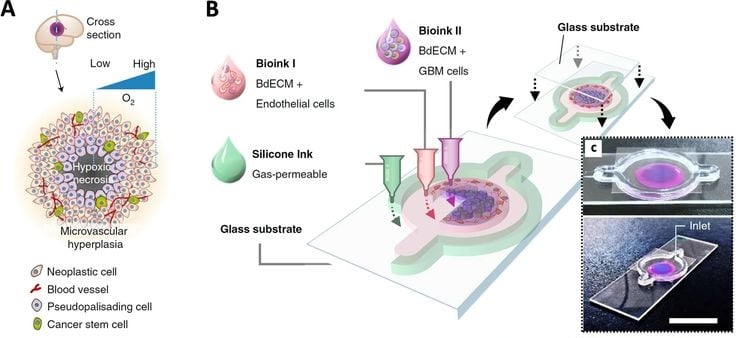
a) Schematic representation of a tumor cross-section depicting the hypoxic core and different biological components typically found in a tumor microenvironment. b) Schematic illustration of the bioinks used to fabricate a compartmentalized GBM-on-a-chip model. c) Mock representation of bioink compartments of brain dECM laden with HUVECs (depicted in magenta), and brain dECM with GBM cells (blue) shown from above (top) and from the corner (bottom; scale bar, 2 cm).
Image Source: Datta Pet al. 3D Bioprinting for Reconstituting the Cancer Microenvironment. npj Precis. Onc. 4, 18 (2020). Open access.
A recent publication by Jiang et al. described a droplet-based bioprinter that used Matrigel® droplets with cells from lung, kidney, and/or stomach tumors.33 Once deposited in 96-well plates, tumor organoids formed rapidly, in one week, with high inter-organoid homogeneity, and could be powerful for reproducible drug testing. An extrusion-based bioprinting method that deposits cells into an immersion bath made of gelatin has also been successfully used for drug screening.34 This method has been used with patient-derived glioblastoma and fibrosarcoma samples in a 96-well format.35
Microfluidic platforms
3D microfluidic devices are another new platform for culturing tumor cells that uses small volumes and spaces in a network of channels. Using these devices can help make tumor spheroid and organoid sizes more homogenous.36 Many 3D cell culture models grown in microfluidic devices closely mimic the in vivo tumor microenvironment, migration, invasion, and metastasis. Microfluidic platforms can differ in the material, scaffolds, and cell types used.15In addition, automated, high-throughput drug screening platforms that use microfluidic devices have recently been developed by Schuster et al.37 The platform was used to test monotherapy, combinatorial, and sequential treatment regimens on patient-derived pancreatic ductal adenocarcinoma organoids. While the platform could mimic many aspects of in vivo tumor physiology, it still suffers from some of the major drawbacks of these devices: The cost and need for a multi-disciplinary team to run drug screening protocols.
closing the translation gap: the shift from 2d to 3d cancer models
The shift from conventional 2D cell cultures to advanced 3D cell culture models marks a significant stride toward more accurate pre-clinical modeling that may translate to the clinic. In the short term, 3D cell cultures will complement using 2D monolayer cultures in preclinical testing. The continued development of more sophisticated and reliable 3D cell culture models is key to narrowing the translation gap, offering a secure bridge between in vitro and in vivo studies that is essential for the success of oncology drug discovery and development. As the field progresses, the integration of 3D cell cultures into preclinical research is poised to revolutionize how drug developers approach and understand cancer therapeutics.
ADvanced 3d cell culture model development at certis oncology
Certis Oncology develops 3D tumor spheroid models from patient-derived xenografts (PDX). These organoid-like structures complement traditional preclinical drug discovery and development approaches, such as pharmacological testing using 2D cell cultures and animal studies.
Consistency is key: a Paired in vitro-to-in-vivo Platform
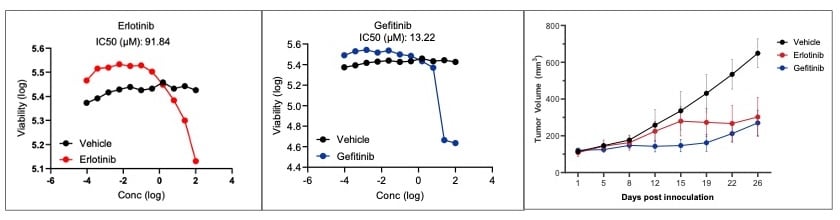
In a recent Certis Oncology proof-of-concept study, two antineoplastics approved to treat advanced non-small cell lung cancer (NSCLC) were screened against a tumor spheroid model developed internally (BarneyOI® Cancer Model CRT00295). In vitro and in vivo pharmacology testing results were compared using the matched PDX model. The half-maximal inhibitory concentration values showed that the tumor spheroid model was highly concordant with in vivo pharmacology results. These results highlight the power of tumor spheroid models and the benefits of having matched PDX-derived 3D cell cultures and mouse models. Armed with advanced matched pairs, drug developers can cross-validate in-vitro-to-in-vivo study results, saving time and money by pursuing the most attractive drug candidates. Image Source: Data on File (2024).
LEARN MORE ABOUT 3D Cell Cultures & matched pairs for preclinical development
References
- Wong CH et al. Estimation of Clinical Trial Success Rates and Related Parameters. Biostat Oxf Engl. 2019;20(2):273-286.
- Jensen C et al. Is It Time to Start Transitioning From 2D to 3D Cell Culture? Front Mol Biosci. 2020;7.
- Kapałczyńska M et al. 2D and 3D Cell Cultures – A Comparison of Different Types of Cancer Cell Cultures. Arch Med Sci AMS. 2018;14(4):910-919.
- Booij TH et al. 3D Cell-Based Assays for Drug Screens: Challenges in Imaging, Image Analysis, and High-Content Analysis. Slas Discov. 2019;24(6):615-627.
- Elliott NT et al. A Review of Three-Dimensional In Vitro Tissue Models for Drug Discovery and Transport Studies. J Pharm Sci. 2011;100(1):59-74.
- Soares CP et al. 2D and 3D-Organized Cardiac Cells Shows Differences in Cellular Morphology, Adhesion Junctions, Presence of Myofibrils and Protein Expression. PLOS ONE. 2012;7(5):e38147.
- Ben-David U et al. Genetic and Transcriptional Evolution Alters Cancer Cell Line Drug Response. Nature. 2018;560(7718):325-330.
- Gomez-Roman N et al. A Novel 3D Human Glioblastoma Cell Culture System for Modeling Drug and Radiation Responses. Neuro-Oncol. 2017;19(2):229-241.
- Aljitawi OS et al. A Novel 3 Dimensional Stromal-Based Model for In Vitro Chemotherapy Sensitivity Testing of Leukemia Cells. Leuk Lymphoma. 2014;55(2):378-391.
- Ramaiahgari SC et al. A 3D In Vitro Model of Differentiated HepG2 Cell Spheroids with Improved Liver-Like Properties for Repeated Dose High-Throughput Toxicity Studies. Arch Toxicol. 2014;88(5):1083-1095.
- Verjans ET et al. Three-Dimensional Cell Culture Models for Anticancer Drug Screening: Worth the Effort? J Cell Physiol. 2018;233(4):2993-3003.
- Antoni D et al. Three-Dimensional Cell Culture: A Breakthrough in Vivo. Int J Mol Sci. 2015;16(3):5517-5527.
- Chen KY et al. Single-Cell Transcriptomics Reveals Heterogeneity and Drug Response of Human Colorectal Cancer Organoids. Conf Proc IEEE Eng Med Biol Soc. 2018;2018:2378-2381.
- Costa EC et al. 3D Tumor Spheroids: An Overview on the Tools and Techniques Used for Their Analysis. Biotechnol Adv. 2016;34(8):1427-1441.
- Jubelin C et al. Three-Dimensional In Vitro Culture Models in Oncology Research. Cell Biosci. 2022;12(1):155.
- Gunti S et al. Organoid and Spheroid Tumor Models: Techniques and Applications. Cancers. 2021;13(4):874.
- Quereda V et al. A Cytotoxic Three-Dimensional-Spheroid, High-Throughput Assay using Patient Derived Glioma Stem Cells. SLAS Discov Adv Life Sci R D. 2018;23(8):842-849.
- Halfter K et al. Testing Chemotherapy Efficacy in HER2 Negative Breast Cancer Using Patient-Derived Spheroids. J Transl Med. 2016;14:112.
- Jeppesen M et al. Short-Term Spheroid Culture of Primary Colorectal Cancer Cells as an In Vitro Model for Personalizing Cancer Medicine. PLoS ONE. 2017;12(9):e0183074.
- Nunes AS et al. 3D Tumor Spheroids as In Vitro Models to Mimic In Vivo Human Solid Tumors Resistance to Therapeutic Drugs. Biotechnol Bioeng. 2019;116(1):206-226.
- Árnadóttir SS et al. Characterization of Genetic Intratumor Heterogeneity in Colorectal Cancer and Matching Patient‐derived Spheroid Cultures. Mol Oncol. 2018;12(1):132-147.
- Minchinton AI et al. Drug Penetration in Solid Tumours. Nat Rev Cancer. 2006;6:583-592.
- Friedrich J et al. Spheroid-Based Drug Screen: Considerations and Practical Approach. Nat Protoc. 2009;4(3):309-324.
- Ryu NE et al. Spheroid Culture System Methods and Applications for Mesenchymal Stem Cells. Cells. 2019;8(12):1620.
- Jacob F et al. A Patient-Derived Glioblastoma Organoid Model and Biobank Recapitulates Inter- and Intra-tumoral Heterogeneity. Cell. 2020;180(1):188-204.e22.
- Li X et al. Oncogenic Transformation of Diverse Gastrointestinal Tissues in Primary Organoid Culture. Nat Med. 2014;20(7):769-777.
- Maenhoudt N et al. Developing Organoids from Ovarian Cancer as Experimental and Preclinical Models. Stem Cell Rep. 2020;14(4):717-729.
- Neal JT et al. Organoid Modeling of the Tumor Immune Microenvironment. Cell. 2018;175(7):1972-1988.e16.
- Gilazieva Z et al. Promising Applications of Tumor Spheroids and Organoids for Personalized Medicine. Cancers. 2020;12(10):2727.
- van de Wetering M et al. Prospective Derivation of a Living Organoid Biobank of Colorectal Cancer Patients. Cell. 2015;161(4):933-945.
- Xie X et al. Tumor Organoid Biobank-New Platform for Medical Research. Sci Rep. 2023;13(1):1819.
- Zhao Z et al. Organoids. Nat Rev Methods Primer. 2022;2(1):1-21.
- Jiang S et al. An Automated Organoid Platform with Inter-organoid Homogeneity and Inter-patient Heterogeneity. Cell Rep Med. 2020;1(9):100161.
- Germain N et al. Current Advances in 3D Bioprinting for Cancer Modeling and Personalized Medicine. Int J Mol Sci. 2022;23(7):3432.
- Maloney E et al. Immersion Bioprinting of Tumor Organoids in Multi-Well Plates for Increasing Chemotherapy Screening Throughput. Micromachines. 2020;11(2):208.
- Wu LY et al. Microfluidic Self-Assembly of Tumor Spheroids for Anticancer Drug Discovery. Biomed Microdevices. 2008;10(2):197-202.
- Schuster B et al. Automated Microfluidic Platform for Dynamic and Combinatorial Drug Screening of Tumor Organoids. Nat Commun. 2020;11:5271.
ABOUT THE AUTHOR
Elie Diner has a PhD in bioengineering and 12 years of research experience in microbiology, synthetic biology and immunology. During his time at the bench, he developed a passion for effective science communication and eventually transitioned into a career as a professional science and content writer. He's authored 12 peer-reviewed scientific publications and numerous blogs, whitepapers, and eBooks for life science companies.
Back to Feed

